
As more and more of Picto’s clients ask for signage and wayfinding that takes into account the needs of people living with dementia and which sees dementia design integrated into mainstream projects, so Picto continue to explore the current thinking on this topic.
Joining a group of UK and international design professionals who are working – or have worked – on dementia-specific design projects, Sarah Phillips attended the two-day design school, The Intersection of Dementia + Design, hosted by RIBA London and run by the Dementia Services Development Centre (DSDC) at Stirling University.
Attending the course was a practical way to gain a better understanding of dementia, the issues that surround it and the challenges it presents. It was also an opportunity to find out more the role that design – and by association, signage and wayfinding – has to play in helping people who are living with a diagnosis of dementia.
Why The Intersection of Dementia + Design?
An architect and a dementia social care practitioner led the course over the two days. They worked together to highlight that it is through the intersection of their disciplines – design and social care – that a positive and significant impact can be made upon those who live with the condition.
They explained that dementia could take over 200 forms, and therefore different people can experience their diagnosis in very different ways. For example, a common symptom of dementia is a worsening of vision, which can make it difficult for people to discriminate between colours. This is clearly of critical importance when developing wayfinding and signage.
What is the current thinking around to dementia design?
Over the two days, it was revealed that most of the current thinking around dementia and design focuses on health and social care environments, with an emphasis on making spaces feel welcoming and homely.
We heard that research is showing how the use of design elements can help people with early-onset dementia to stay in their own homes for as long as possible and how well designed spaces can reduce:
– Confusion and agitation
– The use of medication in dementia patients
– The number of falls
– Diagnoses of depression
And improve a person’s:
– Ability to cope with their diagnosis
– Ability to continue living a fulfilling life
– Physical fitness
– Ability to find their way
The NHS is already recognising the role that design plays in supporting people living with dementia, and how the application of best practice principles can improve patient outcomes and save money. With the current cost to the NHS of falls due to visual impairment (which may or may not be linked to dementia) standing at £269 million a year, the role that design can play in keeping people safe is of great importance.
Research is also showing that hospitals are one of the worst environments for patients living with dementia because they can trigger a rapid decline in patient health. As a result, there is currently a focus on actively improving spaces in these care environments, as well as a push to include dementia-specific design as standard in new care developments.
Sensory considerations as an element of dementia design
As well as affecting people’s vision, dementia can also affect the other senses. Sensory overload is a common cause of added confusion, and so, when it comes to design, it is important that this is considered.
• Hearing – it can be difficult for people with dementia to filter out background noise, so the ability to control noise levels is critical.
• Vision – dementia can have a severe impact on people’s sight, and visual overload may cause some people living with dementia to become agitated and feel stressed.
A consideration to avoid this could be that walls in interior spaces are left neutral, while patterns can be considered and introduced in such a way as to make them easy to remove or change if they are found to be too stimulating for a particular person.
This means that, rather than creating plain and neutral living spaces as standard, patterns can be introduced with soft furnishings.
• Smell and taste – the smells and tastes of everyday things can be used to stimulate memories, for example, the smells cooking and baking.
Smells can also be used to support orientation – for example, to help signify the location of a dining room within a social care facility.
• Touch – additional touch can help to make up the loss of stimulation from other senses.
This might be in the form of one-to-one contact from a carer, via pet therapy or the use of support aids like grab rails, which can be textured to make them more tactile and pleasing to the touch.
Dementia design as bespoke design
The course leaders emphasised that, when it comes to dementia design, what might be helpful for one person living with dementia, might be unhelpful and even confusing for another. This consideration relates to both the design of the environment and the care that is received.
An example of the need for this consideration would be in a residential facility, where Picto can be asked to specify the means for displaying a photograph as part of a room signage scheme, generally alongside a numbering system.
The consideration here, then, is who is the photograph for? Is it to help the person whose room it is, or is it to help the staff and visitors to know who lives in which room?
In addition to this is the question of what photographs would be the most helpful to the person whose room it is, to help them find their way back? For some people with dementia a current photograph would work, whereas for others, it may need to be a photo from when they were younger. Or perhaps, depending on the person’s memory, it may need to be a combination of the two.
The introduction of this explanation highlighted that for some people living with dementia, their reality could be set at a time in the past. The example given was of Ronald Reagan who, when he was living with dementia, remembered neither when he was an actor nor when he was the President of the United States. Instead, he recalled being a lifeguard as a young man – and identified with that time in his life.
The intersection of dementia + design
The preservation of longer-term memories in people living with dementia can explain the positive impact that design elements from the past can have when used in care environments. Such items feel familiar, and the person living with dementia can remember how to use them. For social care spaces, then, playing music from the past or keeping memory boxes in resident’s rooms, can be helpful in stimulating both conversation and memories.
The positive contribution of design
One of the most interesting aspects of the course was the role that design can have in making a positive contribution to the lives of people living with dementia, from simple changes in the home environment to specifically-designed health and social care spaces.
Helpful design elements include:
• Spatial layouts that avoid dead ends and enable people to move freely between rooms
• Spaces with specific and well-defined functions, like dining areas and living areas, which can aid orientation and wayfinding
• The use of appropriate objects, like a watering can in a garden area or magazines and jigsaws in a living room to help people locate themselves within a space
• Artwork can be used to aid recognition and as a source of sensory stimulation
• Unobtrusive safety features
The role of colour in dementia design
Colour plays an essential role in dementia design. Ensuring good light reflective value (LRV) levels between the colour of walls, furniture and flooring is critical to creating a safe environment as it means surfaces are easier to identify.
The use of objects, like quirky door stops or eye-catching artwork, can function as landmarks to aid orientation, replacing the more traditional colour coding that may not be helpful for people whose sight and ability to differentiate between colours has been affected by their diagnosis.
Care is needed with decorative elements like feature walls incorporating large format graphics or scenic wallpapers featuring life sized elements like bookcases or drawers – all of which can cause confusion and create feelings of disorientation.
Seemingly simple things like coloured toilet seats and grab rails can allow people to retain their dignity and support their continuing independence. As demand for these products increases, so manufacturers are improving the products and finishes that are available and there is increasing choice on the market.
Signage needs to work with all of these elements, and so careful planning is required to ensure all of the LRVs work together and meet with the minimum guidelines set by Stirling University.
Historically, yellow was thought to be the best colour for signage in dementia design. It’s now known that, as long as the light reflective values of a sign are at the levels required for clarity and ease of differentiation, we can consider a full-colour palette.
The importance of outside space
A connection with and access to outdoor spaces, particularly in social and healthcare settings, is extremely valuable for people living with dementia. Being able to get outside in the fresh air and daylight has many benefits to improving and maintaining health.
In design terms, this means that windows should be positioned to have unobstructed views of any outside spaces and without a mullion line at eye level – particularly in relation to the position of a bed in a bedroom.
The role of interior and exterior lighting design
People living with dementia need a lot of light to be able to make sense of their environment. Light affects everyone’s circadian rhythms, which are the physical, mental, and behavioural changes that follow our daily cycle and which respond primarily to light and darkness.
For people living with dementia, the disruption of these rhythms can have a dramatic effect on sleep patterns, levels of agitation and appetite.
This means that lighting plays a critical support role for people living with dementia, which can be hard to meet during the winter months when the weather can restrict the available amount of natural daylight.
However, recent developments in lighting technology mean that some types of internal lighting can now almost replicate daylight. This can compensate for a lack of natural light if a person living with dementia is unable to go outside due to during periods of severe weather or poor health.
As commercial demand for such lighting increases, so lighting manufacturers recognise an emerging need and develop new products.
The role of exterior space design
One particular highlight of the course was learning how access to daylight can help to regulate the circadian rhythms, which is particularly important for people living with dementia. An added benefit of access to daylight and outside space is the opportunity for exercise and social interaction, fresh air and the stimulation provided by engaging with nature.
Being able to walk freely in a safe space is important in supporting people living with dementia, especially in the mid-to-late stages of the disease when sundowning – an increased restlessness late in the day – can be a common symptom.
It was emphasised on the course how spaces that incorporate doors that can’t be unlocked and opened and which prevent people from going outside can provoke feelings of stress and frustration.
In contrast, well designed outside spaces can provide stimulation and aid faster recovery from illness, reducing both stress and promoting lower blood pressure.
As part of the course, all the participants took part in an exercise to design an engaging and dementia-friendly garden to fit the space on the rooftop at RIBA HQ. We learned how specific design elements, including planting schemes, spatial layouts and handrails, could keep people in the advanced stages of dementia safe in enclosed garden spaces, concealing dangerous elements and deterring people from exploring unsafe areas.
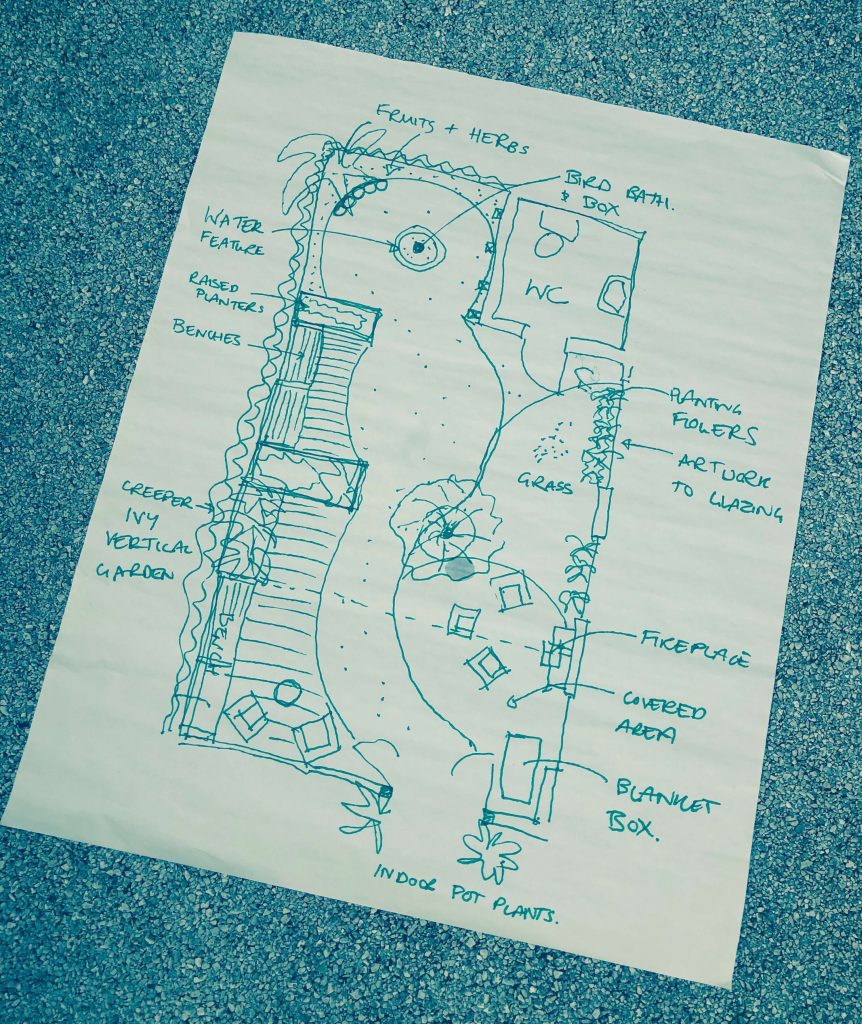
Sketch of our design for a dementia friendly garden, based on the space on the RIBA rooftop, incorporating elements to engage with, safety features such as handrails and for added comfort a blanket box. Indoor pot plants positioned at the entrance to the garden act as a navigation aid and provide a cue as to what is through the doors.
Thoughts and reflections
When working on any wayfinding project, I always try and put myself in the shoes of the people who need to navigate that space. What this course showed me was that everyone who lives with dementia experiences his or her diagnosis differently.
Completing the course has made me think about projects in a new way. I have a better understanding of dementia and the issues that surround people who are living with a diagnosis – and a set of principles to be able to draw upon when I’m developing wayfinding schemes.
As always, the subject of toilet signage was of particular interest to us at Picto. We know that supporting people to be able to locate and use the toilet is an integral part of helping them to retain their dignity and, at this part of the course, our interest focused around the physical placement of signs to indicate toilet facilities for people living with dementia. Current learning includes the use of words and recognisable images in toilet signage, as well a consideration of as where and how toilet signs should best be located and treated within the interior colour scheme.
I was pleasantly surprised that there’s much more current thinking about the signage element of dementia-specific design than I expected. The fact that much of the current thinking around dementia design focuses upon its application in social care or healthcare environments is evolving as research in other types of buildings, including community facilities and airports is carried out.
Since completing the course, I find I’m having more informed conversations with my clients, colleagues and my peers and know that we have to prepare to be frustrated – simply because there isn’t always an answer – or not yet. But we do have a range of ways to work, and by staying up-to-date on developments and by collaborating – we can continue to make a positive difference.
It’s provoked a lot of thinking, both for the here and now, and the future. On a simple level, how will we make mainstream buildings interesting and appealing to everyone, while taking into account an awareness of dementia design? And what do we need to do to keep up with the latest developments and research in the field?
At Picto, we’re now exploring ways to keep our knowledge of dementia design up-to-date so that we can apply the principles to client projects, across all sectors.
Sarah Phillips, July 2018





